
Malaria infects more than 250 million people a year and kills almost one million — most of them children. The disease is curable with the right treatment, but this year scientists announced that it may not be curable for long. Strains of malaria that have evolved resistance to our most effective drug, artemisinin, have been discovered in western Cambodia and could spread to the rest of the world. Understanding the environment that contributed to this worrisome evolutionary step is helping scientists, doctors, and policymakers develop effective strategies for keeping resistant strains of malaria in check.
Where's the evolution?
At the most basic level, resistance is an evolutionary phenomenon: All populations — including populations of disease pathogens — have genetic variation. Some individuals have the genes to handle particular environmental stresses and opportunities better than others. And when the population is exposed to a stress, the individuals that happen to carry the right mutated genes survive and reproduce at higher rates. Over many generations, individuals carrying the helpful mutations will become more frequent in the population. This is basic natural selection at work, and just as it shapes birds’ beaks to take advantage of available seed sizes, it favors the evolution of pathogen populations that can resist the drugs in their environments.
Scientists now have evidence that this is exactly what has happened in western Cambodia — and it has them worried for several reasons. First, artemisinin is the most effective malaria drug we have left. The malaria pathogen, Plasmodium falciparum has already evolved resistance to other drugs like chloroquine. Second, Cambodia seems to be a harbinger of malaria resistance. Resistant malaria strains frequently crop up in Cambodia before spreading to the rest of the world. If artemisinin-resistant malaria strains become established in Cambodia and then spread, malaria deaths will likely skyrocket.
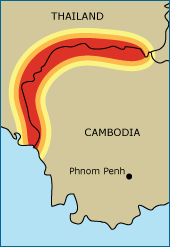
What’s going on in Cambodia that makes it such a hotbed for the evolution of resistance? To understand, you first need to know the evolutionary reasoning behind combination drug therapies. Combination therapies are one of the ways that doctors and medical researchers plan for — and try to prevent — evolution in pathogens. It works like this. If you use just drug A to treat a person infected with a particular pathogen, there’s a fair chance that some individual in the pathogen population will happen to carry a mutation that gives it resistance to drug A and that allows it to start a new resistant strain as it reproduces. Drug B used alone has the same drawback. But it’s extremely unlikely that any single pathogen would happen to carry mutations conferring resistance to both drugs A and B. If you treat the infected person with both drugs at the same time — an approach known as combination therapy — any pathogen that doesn’t get wiped out by one drug is likely to be halted by the other. By killing or stopping the reproduction of all the individual pathogens infecting a person, combination therapy doesn’t give the pathogen population a chance to evolve into a resistant strain.
Societal issues in western Cambodia make it difficult to get people treated with the combination therapies they need. Many Cambodians buy their drugs from local dealers on a pill-by-pill basis. This means that many opt to buy just the artemisinin pill, without the appropriate partner drug (e.g., mefloquine) — especially since those partner drugs have side effects like headaches, seizures, and even hallucinations and since artemisinin acts quickly to improve malaria symptoms. Pill-by-pill purchases also make it less likely that people will stick to their drug regimens long enough to kill all the malaria parasites infecting them, providing even more opportunities for resistant strains to evolve. Furthermore, the black market is rife with substandard malaria treatments and underdoses — additional factors that favor the evolution of resistant strains. Combination malaria therapy is actually required by law in Cambodia, but few get the appropriate treatment. It’s no surprise then that resistant malaria strains tend to pop up in western Cambodia — and when they do, they spread to other places, carried by migrants who work in the Cambodian gem mines.
The threat of widespread artemisinin-resistant malaria is dire, but not inevitable. The global medical community responded to this threat last month by launching a new program to make combination therapies available in Cambodia and a few other regions at hugely reduced prices. The program will make doing the right thing to prevent the evolution of resistant malaria strains the cheapest option. If it is successful, it will let us keep artemisinin as an effective treatment and, medical workers hope, wipe out malaria entirely in regions where resistant strains tend to evolve.
News update, July 2012
Since artemisinin-resistant malaria was first discovered in Cambodia in 2009, scientists have been studying this tough-to-kill parasite strain, hoping to find the key to combat it — or at least control its spread. In April of this year, an international research team announced that they’d made major progress towards that goal by identifying the region of the parasite’s genome that is responsible for its drug resistance.
How did the team pinpoint this region? Using evolutionary reasoning. They looked for evidence of what is called a “selective sweep” — the rapid spread of an advantageous mutation. To understand how selective sweeps work, consider this hypothetical example. Imagine that a new advantageous mutation occurs on Chromosome 4, right next to gene sequences coding for black hair and bushy eyebrows. The mutation and those gene versions are physically linked. Because the new mutation is so advantageous, its carrier leaves lots of offspring — many of whom carry the mutation, as well as the linked gene versions. If the advantageous mutation spreads through the population quickly, recombination will not have time to break up the mutation/bushy eyebrows/black hair combination. In the end, a large portion of the population might wind up carrying the genes for black hair and bushy eyebrows, even though these traits are not particularly advantageous. A side effect of this selective sweep is that in this region of the genome, the population will have very low levels of variation because almost everyone carries the same gene versions.
The researchers reasoned that since artemisinin is the most common drug used to treat malaria, artemisinin resistance would be an extremely advantageous mutation for malaria parasites and would have risen to high frequency in the parasite population through a selective sweep. Hence, they compared the genomes of parasites from resistant populations and parasites from non-resistant populations looking for regions with very low levels of variation — one of the hallmarks of a selective sweep. Using this technique they identified several regions of the genome that had experienced recent positive selection — but which was responsible for artemisinin resistance? To narrow in on the genetic culprit, the scientists figured out which of the genetic signatures in these regions had risen in frequency during the spread of resistance on the Thai-Burmese border: a small section of chromosome 13.
The team has yet to figure out exactly which mutation in this region is responsible for the parasite’s resistance, but that’s their next target. Stay tuned for further updates!
Primary literature:
- Cheeseman, I. H., Miller, B. A., Nair, S., Nkhoma, S., Tan, A., Tan, J. C., ... Anderson, T. J. C. (2012). A major genome region underlying artemisinin resistance in malaria. Science. 336: 79-82. Read it »
- Dondorp, A. M., Nosten, F., Yi, P., Das, D., Phyo, A. P., Tarning, J., Lwin, K. M., et al. (2009). Artemisinin resistance in Plasmodium falciparum malaria. New England Journal of Medicine 361(5):455-467. Read it »
- Enserink, M. (2008). Malaria: signs of drug resistance rattle experts, trigger bold plan. Science 322(5909):1776. Read it »
News articles:
- A news article on recent efforts to halt resistant strains of malaria from TIME
- A slide show on advances in malaria research and treatment from Scientific American
- An overview of the evolution of drug resistance from the New York Times
Understanding Evolution resources:
- Imagine that you read a news article that explains that “malaria is growing resistant to our drugs.” Do you think this is a clear way to explain the problem? Why or why not? If not, how would you describe the problem?
- The evolution of drug resistance involves three “steps”: variation, differential reproduction, and heredity. (See our tutorial on natural selection for a review.) Which of these steps does combination therapy cut short? Does it change the variation in the population, affect differential reproduction, or alter heredity? Explain your reasoning.
- Do some research online and find examples of at least two other diseases that are treated with combination drug therapies to prevent or slow the evolution of resistance.
- Imagine that a friend of yours lives in Central America, where artemisinin is effectively used to treat malaria. Should she be worried about the evolution of artemisinin-resistant strains of malaria in Cambodia — a whole continent away? Explain why or why not.
- Farmers and agricultural scientists are often concerned about pests evolving resistance to their pesticides. Describe a “combination therapy” approach to tackling this problem. Do you think it would work? Explain your reasoning.
- Teach about the evolution of antibiotic resistance (select the Marc Lipsitch video): In this 39 minute video for AP biology students, Professor Marc Lipsitch explains how bacteria evolve resistance and why this poses such a threat.
- Teach about natural selection and resistance: In this activity for grades 9-12, students learn why evolution is at the heart of a world health threat by investigating the increasing problem of antibiotic resistance in such menacing diseases as tuberculosis.
- Teach about computer modeling and antibiotic resistance: This article for grades 9-12 examines how the scientist Carl Bergstrom uses computer modeling to understand and control the evolution of antibiotic resistant bacteria in hospitals.
- Teach about evolutionary medicine: This chapter for advanced high school students or undergraduates is excerpted from Carl Zimmer's evolutionary biology textbook, The Tangled Bank. It describes how evolutionary biology informs and advances medical science. It is reprinted with the permission of Roberts and Company Publishers, Inc.
- Cheeseman, I. H., Miller, B. A., Nair, S., Nkhoma, S., Tan, A., Tan, J. C., ... Anderson, T. J. C. (2012). A major genome region underlying artemisinin resistance in malaria. Science. 336: 79-82.
- Dondorp, A. M., Nosten, F., Yi, P., Das, D., Phyo, A. P., Tarning, J., Lwin, K. M., et al. (2009). Artemisinin resistance in Plasmodium falciparum malaria. New England Journal of Medicine 361(5):455-467.
- Enserink, M. (2008). Malaria: signs of drug resistance rattle experts, trigger bold plan. Science 322(5909):1776.
- Enserink, M. (2009). Taking aim at parasites — and drug resistance. ScienceNOW. Retrieved November 23, 2009 from ScienceNOW
- Shay, C. (2009). In malaria hotspot, resistance to a key drug. TIME Magazine. Retrieved November 23, 2009 from TIME Magazine
- Vogel, G. (2009). Ground zero for malaria drug resistance? ScienceNOW. Retrieved November 23, 2009 from ScienceNOW
