 It’s that time of year again. Coughing coworkers, student absences, and reminders to get your shot are sure signs that flu season is upon us. This year’s epidemic seems to have struck earlier and harder than usual — all amid concerns over shortages of the flu vaccine. While some vaccines provide lifelong protection with one or a few doses (e.g., measles, mumps, and polio), the flu requires a new shot every year. And in some years, the flu shot is hardly effective at all. Why is the flu vaccine different from so many other vaccines? A look at the evolution of the flu virus can explain the weaknesses of current vaccines and points the way towards a vaccine that could provide long-lasting, universal protection.
It’s that time of year again. Coughing coworkers, student absences, and reminders to get your shot are sure signs that flu season is upon us. This year’s epidemic seems to have struck earlier and harder than usual — all amid concerns over shortages of the flu vaccine. While some vaccines provide lifelong protection with one or a few doses (e.g., measles, mumps, and polio), the flu requires a new shot every year. And in some years, the flu shot is hardly effective at all. Why is the flu vaccine different from so many other vaccines? A look at the evolution of the flu virus can explain the weaknesses of current vaccines and points the way towards a vaccine that could provide long-lasting, universal protection.
Where's the evolution?
The basic reason for the difference between the flu vaccine and many other vaccines is that the flu virus evolves much more rapidly than do viruses like measles, mumps, and polio. Our bodies fight off diseases, in part, through the production of antibodies that help our immune systems recognize and attack foreign invaders. Vaccines work by priming the body with the right antibodies to fight a particular disease before it gets a foothold and makes us sick. For measles, mumps, and polio, this works just fine. If you were fully vaccinated for these diseases as a child (or had the disease as a child) and your body encounters one of these pathogens many years later, it is extremely likely that your body’s antibodies will be able to recognize the intruders and attack them. However, the flu evolves so much from season to season that last year’s antibodies usually cannot recognize this year’s viral strain. So if you were vaccinated for flu last year or had the flu last year, it indicates nothing about your body’s ability to fend off the bug this year.
In fact, in a process called antigenic drift, flu evolves in response to the antibodies our bodies produce each year. During the course of a flu epidemic, many people gain immunity to the strain of the virus that is currently circulating. Through the process of natural selection, any flu virus particles that happen to carry mutations that allow them to slip by the defenses of common antibodies will be favored, produce more copies of themselves, and eventually, spread to more new victims. This process leads to the evolution of new strains, one or some of which are likely to become the cause of next year’s flu season.
Each year’s flu vaccine is actually a cocktail of vaccines for a few different flu strains (generally three) that World Health Organization scientists predict will spread during that year’s flu season. Usually, the predictions match the most common strains closely enough that the vaccine ends up being fairly effective. (This year’s vaccine provides about 60% increased protection for those who are vaccinated.) Very occasionally, however, the most common strains are unexpected ones, and getting a flu shot does little to stave off the disease.
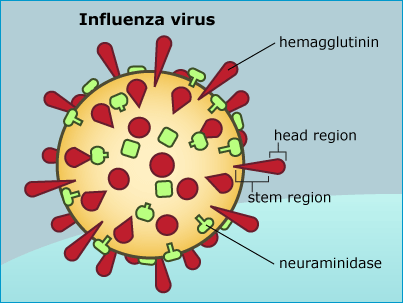 Now, many researchers think that a new approach to the flu vaccine could make it more consistently effective and alleviate the need to get a shot every year. Current vaccines produce antibodies that recognize a protein on the outer coating of the virus called hemagglutinen, and they focus on a particular part of that molecule, the “head” region. The head of hemagglutinen is good at stimulating the production of protective antibodies, but it is also the part of the virus that is most susceptible to antigenic drift. What if researchers could build a vaccine that targeted a part of the flu virus that evolves more slowly?
Now, many researchers think that a new approach to the flu vaccine could make it more consistently effective and alleviate the need to get a shot every year. Current vaccines produce antibodies that recognize a protein on the outer coating of the virus called hemagglutinen, and they focus on a particular part of that molecule, the “head” region. The head of hemagglutinen is good at stimulating the production of protective antibodies, but it is also the part of the virus that is most susceptible to antigenic drift. What if researchers could build a vaccine that targeted a part of the flu virus that evolves more slowly?
Different traits evolve at different rates. For example, traits experiencing strong selection favoring a form different than the current form (as is the case with the head of influenza’s hemagglutinen protein) evolve quickly, while key traits that can’t change much without compromising the functioning of the organism tend to evolve slowly. Slow evolving traits are called evolutionarily conserved traits. It’s easy to understand why very important and finely tuned traits would be conserved. For example, many of the genes that are responsible for laying out the basic body patterns of animals are highly conserved over tens of millions of years of evolutionary history because most mutations to these genes have effects that are incompatible with life and are not passed on.
Many scientists suspect that highly conserved molecules in the flu virus could be used as the basis of a universal flu vaccine that wouldn’t need to be reformulated (and re-received!) every year. A few proteins hold particular promise. First, though the head of hemagglutinen evolves at lightening speed, certain parts of the hemagglutinen stem (the part that connects to the viral membrane and which helps the virus invade cells in the respiratory tract) are nearly identical across a wide range of flu strains. Another relatively invariable protein found in the viral membrane is called M2. It helps control the pH inside virus particles, allowing them to release their RNA into the host cell and take it over. Neuraminidase (shown in the diagram above) helps newly produced viruses break out of a host cell and also varies little from flu virus to flu virus. One of these slow-evolving molecules might make an ideal target for a flu vaccine that protects against a diversity of viral strains.
The days of a yearly flu shot may be numbered. Researchers are pursuing several different approaches to a vastly improved flu vaccine. As described here, some are focused on building vaccines based on evolutionarily conserved regions of the virus; however, others are working on new ways of making the vaccine on short notice, and still others are working on tweaks to existing flu vaccines that would help our bodies mount a stronger defense against the virus. Though the new research holds promise, it will require many years of additional study before new-and-improved vaccines can be established as safe and effective and brought to market. Until then, the Centers for Disease Control and Prevention recommend that you get your yearly flu shot. It’s not perfect, but it’s still the best way to reduce your odds of spending a feverish, achy week with a box of tissues in your lap!
Primary literature:
- Gilbert, S. C. (2012). Advances in the development of universal influenza vaccines. Influenza and Other Respiratory Viruses. DOI: 10.1111/irv.12013. Read it »
- Nabel, G. J., & Fauci, A. S. (2010). Induction of unnatural immunity: prospects for a broadly protective universal influenza vaccine. Nature Medicine. 16: 1389-1391. Read it »
News articles:
- A news article on improving flu vaccines from Boston.com
- A blog post on the topic from the The Scientist
Understanding Evolution resources:
- What role does the process of mutation play in the reformulation of the flu vaccine each year?
- How do the human body’s immune defenses influence the evolution of the flu virus from season to season?
- Review the process of natural selection. Use the four steps described on that page to explain how the hemagglutinen head of a flu strain might evolve over the course of a season.
- Explain the concept of evolutionary conservation.
- Why might some traits be evolutionarily conserved and others might not?
- Read this article about the challenges of developing an HIV vaccine. Compare and contrast these challenges with those of developing a universal flu vaccine. Why are we able to develop a seasonal flu vaccine, but not a seasonal HIV vaccine?
- Teach about rapid evolution and medical applications: In this classroom activity for grades 9-12, students learn why evolution is at the heart of a world health threat by investigating the increasing problem of antibiotic resistance in such menacing diseases as tuberculosis.
- Teach about avian and swine flu: In this article for grades 9-16, students learn about how the flu virus can evolve through gene-swapping, in addition to incremental mutation.
- Teach about HIV vaccine development: In this research profile for grades 9-16, students meet Satish Pillai who studies the evolution of HIV within infected individuals. His research uses the tools of phylogenetics to investigate vaccine development and the possibility of curing the disease.
- Gilbert, S. C. (2012). Advances in the development of universal influenza vaccines. Influenza and Other Respiratory Viruses. DOI: 10.1111/irv.12013.
- Nabel, G. J., & Fauci, A. S. (2010). Induction of unnatural immunity: prospects for a broadly protective universal influenza vaccine. Nature Medicine. 16: 1389-1391.
- Wang, T. T., & Palese, P. (2011). Catching a moving target. Science. 333: 834-835.
