Carl’s work tackles the very real problem of the evolution of antibiotic resistance by bacterial populations in hospitals. Antibiotics, such as penicillin, are drugs that kill or prevent the growth of bacteria. When antibiotics were first discovered, they seemed to represent a miracle cure for human diseases like pneumonia, typhoid, bubonic plague, and gonorrhea. However, almost immediately after the introduction of antibiotics, bacteria began to up the stakes — resistant strains of bacteria soon evolved that could grow even in the presence of a particular antibiotic, rendering our drugs ineffective in battling these resistant infections.
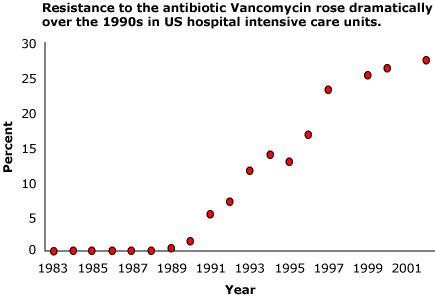
The problem is much like running on a treadmill — medical researchers must sweat just to stay in the same place in their race against the bacteria. Drug companies develop and introduce a new antibiotic, only to see the evolution of resistant bacterial strains within a few years. This necessitates the development of yet another antibiotic, which, in turn, becomes useless in the face of newly evolved resistant bacteria.
The cycle of drug development and the evolution of resistance is a costly one, both in terms of mortality and economics. Over one million resistant infections are acquired each year in U.S. hospitals at an estimated financial cost of 4-5 billion dollars (not to mention increased mortality)! And because they are harder to treat than susceptible infections, antibiotic resistant infections cause more days of hospitalization and missed work. Various sources estimate that in the U.S., we experience 400,000 additional days of diarrhea due to bacterial infections resistant to a single antibiotic alone and more than 8000 additional days of hospitalization due to resistant salmonella strains.
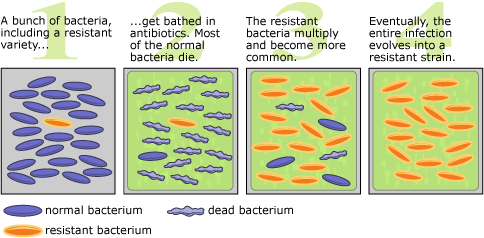
How exactly does antibiotic resistance evolve? How have such small and simple organisms managed to repeatedly outpace our drugs? The process is quite simply evolution by natural selection — but bacteria have a few secret weapons that give them an edge. Imagine a population of bacteria infecting a patient in a hospital. The patient is treated with an antibiotic. The drug kills most of the bacteria but there are a few individual bacteria that happen to carry a gene that allows them to survive the onslaught of antibiotic. These survivors reproduce, passing on the gene for resistance to their offspring, and soon the patient is populated by an antibiotic resistant infection — one that not only affects the original patient but that can also be passed on to other patients in the hospital.
- Learn about how bacteria manage to evolve resistance so quickly: turbo-charged evolution!
- Get tips for using research profiles, like this one, with your students.